Osteoarthritis: Everything You Need to Know!

What is Osteoarthritis?
Osteoarthritis is the most common type of arthritis that affects millions of people around the world. Think of it as the “wear and tear” type of arthritis. To understand this condition better, imagine your joints as door hinges. Over time, these hinges can become rusty and stiff from constant use. Similarly, osteoarthritis happens when the smooth, slippery tissue called cartilage that covers the ends of your bones gradually wears away.
Cartilage acts like a cushion between your bones, allowing them to glide smoothly over each other when you move. When this protective layer breaks down, your bones start rubbing directly against each other. This bone-on-bone contact causes the joint pain, stiffness, and other symptoms that people with osteoarthritis experience.
Healthcare providers sometimes call osteoarthritis “degenerative joint disease” or simply “OA” because it involves the gradual breakdown of joint structures over time. Unlike some other forms of arthritis that affect the whole body, osteoarthritis primarily affects the joints themselves, not your internal organs.
Types of Osteoarthritis
Medical experts classify osteoarthritis into two main types based on what causes it:
Types of Osteoarthritis
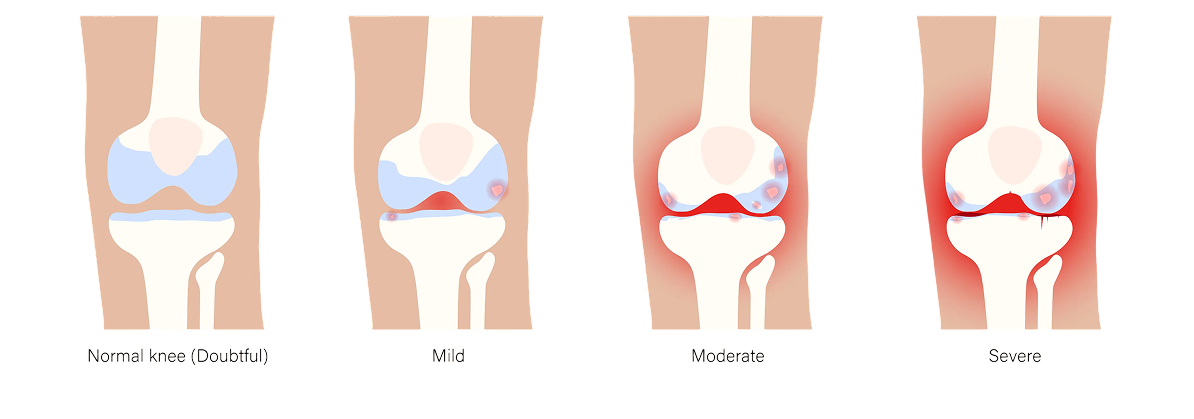
Primary osteoarthritis
Primary osteoarthritis is the most common form. This type develops gradually as you age and use your joints throughout your life. It’s like how the tires on your car slowly wear down from driving – your joints experience normal wear and tear from daily activities like walking, climbing stairs, and using your hands. Most people who develop osteoarthritis have this primary type.
Secondary osteoarthritis
Secondary osteoarthritis occurs when something specific damages your joints enough to cause the condition. This might happen after a sports injury, car accident, or fall that damages the cartilage in a joint. Other types of arthritis, such as rheumatoid arthritis or gout, can also damage joints enough to lead to secondary osteoarthritis later on.
How Common is Osteoarthritis?
Osteoarthritis is extremely common, especially as people get older. Research shows that more than 80% of adults over age 55 have some degree of osteoarthritis, even though not all of them experience noticeable symptoms. About 60% of people with osteoarthritis have symptoms they can feel or notice in their daily lives.
The condition affects people worldwide, with an estimated 240 million people having activity-limiting osteoarthritis globally. In the United States alone, more than 52 million adults have been diagnosed with some form of arthritis, with osteoarthritis being the most prevalent type.
Symptoms and Signs of Osteoarthritis
The symptoms of osteoarthritis typically develop slowly over time and tend to get worse as the condition progresses. Understanding these symptoms can help you recognize when you might need to see a healthcare provider.
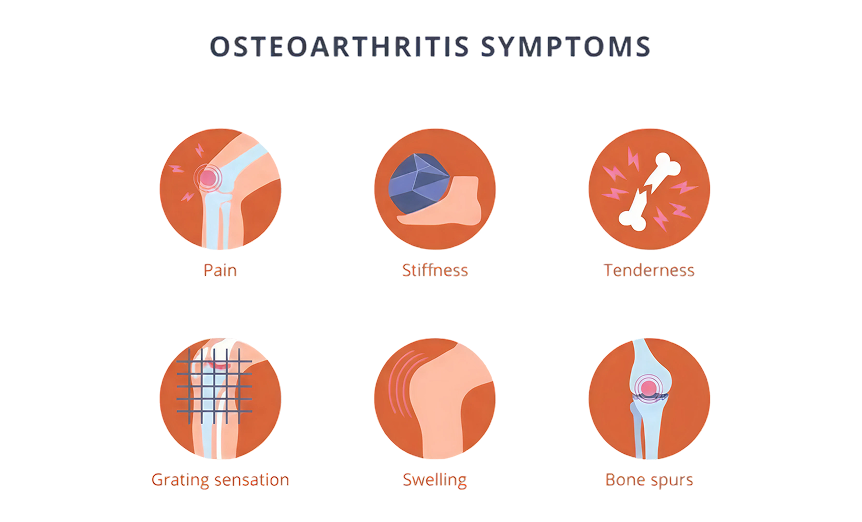
Which Joints Are Most Commonly Affected?
The symptoms of osteoarthritis typically develop slowly over time and tend to get worse as the condition progresses. Understanding these symptoms can help you recognize when you might need to see a healthcare provider.
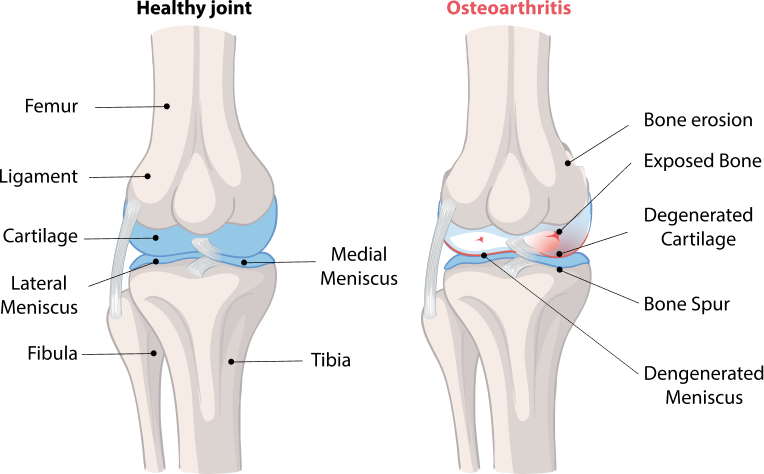
What Causes Osteoarthritis?
While scientists don’t completely understand all the causes of osteoarthritis, they have identified several factors that contribute to its development.
Age is the most significant risk factor. As we get older, our cartilage naturally becomes less elastic and more prone to wear and tear. The water content in cartilage decreases with age, making it more fragile and likely to break down. Additionally, our body’s ability to repair damaged cartilage slows down as we age.
Mechanical stress on joints from daily activities gradually wears down cartilage over time. This is why osteoarthritis is sometimes called a “wear and tear” condition. However, normal activity and exercise don’t cause osteoarthritis – in fact, regular moderate exercise helps keep joints healthy. Here are some of the reasons that are the cause osteoarthritis:
Normal aging
Years of using your joints naturally wear down cartilage
Daily wear and tear
Regular activities slowly damage joint cartilage
Injuries
Sports injuries, falls, or car accidents
Other diseases
Diabetes, high cholesterol, or other types of arthritis
Joint problems
Being born with joint defects
Obesity
Extra weight puts more pressure on weight-bearing joints
How is Osteoarthritis Diagnosed?
Diagnosing osteoarthritis involves several steps, and there’s no single test that can definitively diagnose the condition. Instead, healthcare providers use a combination of your medical history, physical examination, and various tests.
- Medical History: Your doctor will ask detailed questions about your arthritis symptoms, including when they started, what makes them better or worse, and how they affect your daily activities. They’ll also ask about your family history of arthritis, any previous injuries, your occupation, and your overall health.
- Joint examination: During the physical exam, your doctor will look at and feel your joints, checking for swelling, tenderness, warmth, and redness. They’ll test your range of motion by asking you to move your joints in different directions. They’ll also check for joint stability and look for any deformities.
- Imaging Tests help confirm the osteoarthritis diagnosis and assess the severity of joint damage:
- X-rays are the most commonly used imaging test for osteoarthritis. They can show joint space narrowing (indicating cartilage loss), bone spurs (osteophytes), and changes in bone density around the joint. However, X-rays don’t show cartilage directly, so early osteoarthritis might not be visible on X-rays.
- MRI joint imaging provides detailed images of cartilage, ligaments, and other soft tissues around joints. This test is more sensitive than X-rays and can detect early cartilage damage that doesn’t show up on X-rays.
- CT (Computed Tomography) scans may be used in some cases to get detailed images of bone structure and detect subtle changes that might not be visible on regular X-rays.
- Blood tests are usually done to rule out other types of arthritis, such as rheumatoid arthritis or gout, which can have similar symptoms but require different treatments. There’s no specific blood test for osteoarthritis itself.
Joint fluid analysis may be performed if there’s significant swelling in a joint. A small sample of fluid is removed from the joint with a needle and examined under a microscope to check for signs of infection or other types of arthritis.
Treatment and Management Options
While there’s no cure for osteoarthritis, many effective treatments can help manage symptoms, improve joint function, and slow the progression of the disease. Osteoarthritis treatment plans are usually individualized based on which joints are affected, the severity of symptoms, your age, activity level, and overall health.
Non-Medication Treatments
Exercise:
- Low-impact activities: Swimming, walking, cycling
- Strength training: Builds muscles around joints
- Flexibility exercises: Maintain range of motion
- Physical therapy: Professional guidance for safe exercise
Weight Management:
- Losing even small amounts of weight can reduce joint stress
- Every pound lost removes 4 pounds of pressure from the knees
Heat and Cold Therapy:
- Heat: Relaxes muscles and increases blood flow
- Cold: Reduces swelling and numbs pain
Supportive Devices:
- Braces or splints for joint support
- Canes or walkers to reduce weight on joints
- Special shoe inserts for better foot support
Medications
Over-the-Counter:
- Acetaminophen (Tylenol): Good for mild to moderate pain
- NSAIDs: Ibuprofen, naproxen – reduce pain and inflammation
Prescription Medications:
- Stronger NSAIDs
- Topical pain relievers (creams and gels)
- In severe cases, stronger pain medications
Joint Injections
- Corticosteroid injections involve injecting anti-inflammatory medication directly into the affected joint. These injections can provide significant pain relief and reduce inflammation for several months. However, they can only be given a limited number of times per year because repeated injections may damage cartilage.
- Hyaluronic acid injections involve injecting a substance that acts like natural joint fluid into the affected joint. This treatment, sometimes called “viscosupplementation,” may help lubricate the joint and reduce pain. The effects can last for several months.
Complementary and Alternative Therapies
- Acupuncture involves inserting thin needles into specific points on the body. Some studies suggest it may help reduce osteoarthritis pain, particularly in the knee.
- Massage therapy can help reduce muscle tension around affected joints and may provide temporary pain relief.
- Dietary supplements such as glucosamine and chondroitin are popular, though scientific evidence for their effectiveness is mixed. Always talk to your healthcare provider before starting any supplements.
- Mind-body techniques such as meditation, deep breathing exercises, and tai chi may help manage pain and improve overall well-being.
Surgery
Surgery is usually considered only when other treatments haven’t provided adequate relief and symptoms significantly interfere with daily activities.
Arthroscopy is a minimally invasive procedure where a surgeon uses a small camera to look inside the joint and remove damaged cartilage or bone fragments. This procedure is less commonly performed for osteoarthritis than it used to be, as studies have shown limited long-term benefits.
- Joint replacement (Arthroplasty) involves removing the damaged joint and replacing it with an artificial joint made of metal, plastic, or ceramic materials. Hip and knee replacements are the most common and successful joint replacement surgeries. Modern artificial joints can last 20 years or more and can dramatically improve the quality of life for people with severe osteoarthritis.
- Joint fusion (Arthrodesis) involves permanently joining the bones in a joint together. This eliminates joint pain but also eliminates joint movement. This procedure is sometimes used for severely damaged joints in the spine, ankle, or hand.
- Osteotomy involves cutting and reshaping bones to redistribute weight and reduce stress on the damaged part of a joint. This procedure is sometimes used for younger people with osteoarthritis affecting only part of a joint.
How to Live with Osteoarthritis?
Daily Life Tips:
- Pace yourself: Balance activity with rest
- Use larger joints: Carry bags with your arms instead of fingers
- Avoid prolonged positions: Change positions frequently
- Plan ahead: Do harder tasks when you feel best
Home Modifications:
- Install grab bars in bathrooms
- Use lever-style door handles instead of knobs
- Keep frequently used items at easy-to-reach heights
- Use tools with larger, padded grips
Diet and Nutrition:
- Anti-inflammatory foods: Fish, leafy greens, berries
- Maintain a healthy weight: Reduces joint stress
- Stay hydrated: Helps maintain joint lubrication
- Limit processed foods: May increase inflammation
Prevention Tips
What You Can Do:
- Stay active: Regular exercise keeps joints healthy
- Maintain a healthy weight: Reduces joint stress
- Protect your joints: Use proper techniques when lifting
- Wear protective gear: During sports or risky activities
- Don’t smoke: Smoking can worsen arthritis
- Eat well: A balanced diet supports joint health
Complications
If Left Untreated:
- Increased pain: Symptoms typically worsen over time
- Loss of mobility: Difficulty performing daily activities
- Depression: Chronic pain can affect mental health
- Sleep problems: Pain may interfere with rest
- Other health issues: Reduced activity can lead to heart disease, diabetes
When to See a Healthcare Provider?
You should see a healthcare provider if you experience:
Joint pain that lasts more than a few days or keeps coming back. Morning stiffness that lasts more than 30 minutes. Swelling in one or more joints. Difficulty performing daily activities due to joint pain or stiffness. Joint pain that interferes with sleep. Any sudden, severe joint pain or signs of infection, such as fever, redness, or warmth around a joint.
Early diagnosis and treatment can help slow the progression of osteoarthritis and maintain better joint function over time.
How We Can Help You?
At our clinic, we understand that living with osteoarthritis can significantly impact your quality of life. That’s why we offer advanced, cutting-edge treatments that go beyond traditional approaches to help you manage your condition more effectively and potentially slow its progression.
At our clinic, we offer advanced treatment options that go beyond traditional approaches to help manage your osteoarthritis more effectively.
Regenerative Treatments
Platelet-Rich Plasma (PRP) Therapy:
- What it is: We use your own blood, concentrate the healing platelets, and inject them into your affected joints
- How it helps: Platelets contain growth factors that can help repair damaged tissue and reduce inflammation
- Benefits: Natural healing using your body’s own repair mechanisms
- Procedure: Simple blood draw, processing, and injection – usually takes about an hour
Advanced Joint Injections
Hyaluronic Acid Injections:
- Purpose: Replace the natural lubricating fluid in your joints
- How it helps: Reduces friction between bones and may stimulate natural hyaluronic acid production
- Duration: Effects can last 6-12 months
- Best for: Knee osteoarthritis, though it can be used in other joints
Corticosteroid Injections:
- What they do: Powerful anti-inflammatory medications are injected directly into the joint
- Benefits: Quick pain relief and reduced swelling
- Duration: Effects typically last 3-6 months
- Precision: Using ultrasound guidance for accurate placement
Customized Treatment Plans:
- Comprehensive evaluation: We assess your specific condition, lifestyle, and goals
- Combination approach: Often combining different treatments for the best results
- Ongoing monitoring: Regular follow-ups to adjust treatment as needed
- Patient education: Teaching you how to maximize treatment benefits
Why Choose Our Regenerative Approach?
Advantages:
- Minimally invasive: Most procedures are outpatient with minimal downtime
- Natural healing: Using your body’s own healing mechanisms
- Reduced medication dependence: May decrease the need for pain medications
- Improved quality of life: Many patients experience significant improvement in daily activities
- Delayed surgery: May postpone or eliminate the need for joint replacement
What to Expect:
- Initial consultation: Comprehensive evaluation and treatment planning
- Procedure day: Most treatments take 1-2 hours
- Recovery: Minimal downtime, gradual improvement over weeks to months
Follow-up care: Regular monitoring and additional treatments as needed
Getting Started with Our Advanced Treatments
If you’re struggling with osteoarthritis and want to explore these advanced treatment options, we’re here to help. Our team of specialists will work with you to develop a personalized treatment plan that addresses your specific needs and goals.
Contact us today to schedule a consultation and learn how regenerative treatments and advanced joint injections can help you get back to the activities you love.
Remember, early intervention often leads to better outcomes, so don’t wait for your symptoms to worsen. Let us help you take control of your osteoarthritis and improve your quality of life with these cutting-edge treatment options.
Similar Articles
At Conscious Medicine, we understand how debilitating bone-on-bone joint pain can be. Our goal is to reduce pain, improve mobility, and
aLorem Ipsum is simply dummy text of the printing and typesetting industry. Lorem Ipsum has been the industry’s standard dummy text ever since the 1500s, when an unknown printer took a galley of type
- Blog
• ...
- Blog
• PRP works faster (2-6 weeks) with strong evidence for ...
- Blog
• Clinical studies show 70-80% success rates ...


